Mental health care in the USA has seen a remarkable shift over the past decade. With growing awareness, reduced stigma, and expanded insurance coverage, more individuals are seeking therapy and psychiatric services than ever before. But behind every successful mental health practice lies a critical yet often overlooked function—billing for mental health.
Whether you're a solo therapist, a group practice owner, or managing a behavioral health clinic, understanding how billing works can directly impact your revenue, compliance, and patient satisfaction. This guide explores everything you need to know about billing for mental health providers, from coding complexities to outsourcing options and real-world strategies that actually work.
Understanding Billing for Mental Health Providers
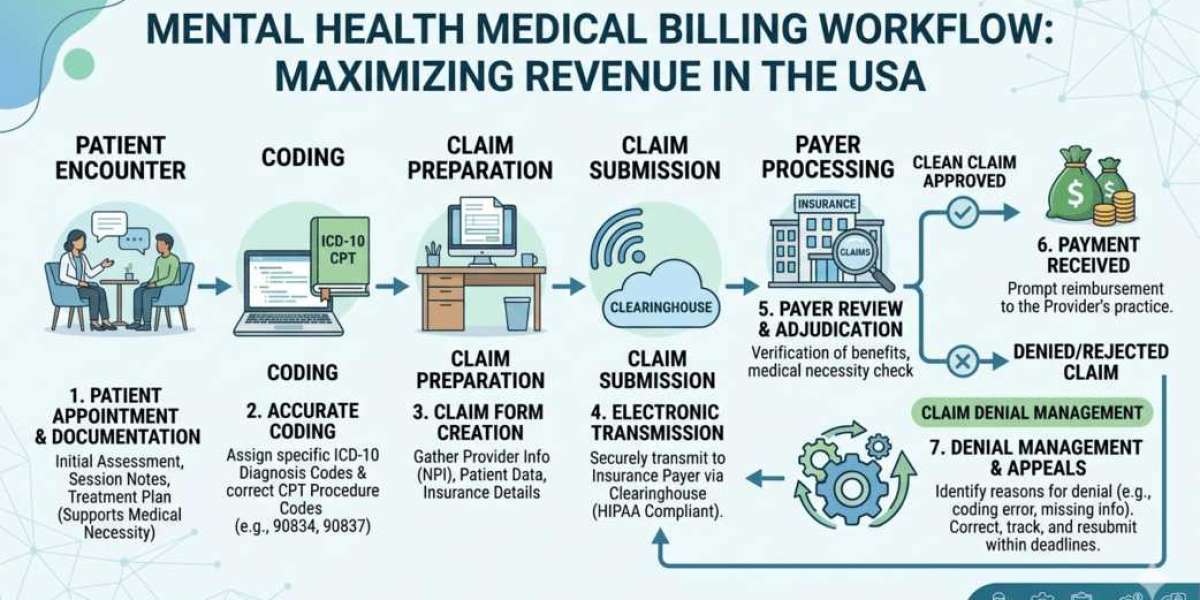
Billing for mental health services is not as straightforward as general medical billing. It involves unique codes, payer-specific rules, and strict documentation requirements. Mental health providers must navigate therapy session durations, telehealth regulations, and varying reimbursement policies.
At its core, medical billing for mental health involves:
- Verifying patient insurance eligibility
- Assigning correct CPT and ICD-10 codes
- Submitting claims to insurance providers
- Following up on denials or rejections
- Managing patient billing and collections
Even a small error in coding and billing for mental health services can lead to claim denials or delayed payments.
Why Mental Health Billing is More Complex Than You Think
Unlike other specialties, mental health billing relies heavily on time-based codes and nuanced documentation. For example, therapy sessions may be billed differently based on whether they last 30, 45, or 60 minutes.
Key Challenges Include:
- Frequent coding updates for behavioral health
- Insurance variability, especially with Medicare and Medicaid
- Authorization requirements for ongoing therapy
- Telehealth billing regulations that change frequently
Because of these factors, many providers struggle to maintain accuracy without specialized support.
Core Components of Mental Health Billing Services
To streamline operations, many clinics rely on professional mental health billing services. These services cover the entire billing lifecycle and reduce administrative burden.
Essential Elements:
1. Insurance Verification
Before any session, verifying benefits ensures the patient is eligible and avoids billing surprises.
2. Accurate Coding
Using proper CPT codes like 90834 or 90837 is critical in billing for mental health therapists.
3. Claims Submission
Timely and clean claim submission improves acceptance rates.
4. Denial Management
Quick identification and correction of denied claims protect revenue.
5. Patient Billing
Transparent billing improves trust and reduces confusion.
Coding and Billing for Mental Health Services: What You Need to Know
Accurate coding is the backbone of mental health medical billing. Without it, even the best clinical care won’t translate into proper reimbursement.
Common CPT Codes:
- 90791 – Psychiatric diagnostic evaluation
- 90834 – 45-minute psychotherapy
- 90837 – 60-minute psychotherapy
- 90853 – Group therapy
ICD-10 Examples:
- F32.0 – Mild depressive episode
- F41.1 – Generalized anxiety disorder
Mistakes in pairing CPT and ICD-10 codes are one of the most common reasons claims get rejected.
Billing Medicare for Mental Health Services
Medicare plays a significant role in mental health coverage, especially for older adults. However, billing Medicare for mental health services comes with strict compliance rules.
Important Considerations:
- Services must be deemed medically necessary
- Providers must be credentialed with Medicare
- Documentation must support treatment plans
- Telehealth rules may differ based on location and policy updates
Failure to comply can result in audits or payment recoupments.
The Role of Credentialing in Mental Health Billing
Before a provider can bill insurance companies, they must complete credentialing. This process verifies qualifications and ensures providers meet payer requirements.
Credentialing Includes:
- License verification
- Education and training validation
- Insurance network enrollment
Without proper credentialing services, providers cannot legally submit claims, making this step essential for revenue generation.
Outsourcing Mental Health Billing: Is It Worth It?
Many clinics are now turning to outsourcing mental health billing to improve efficiency and reduce administrative stress.
Benefits of Outsourced Billing for Mental Health:
- Higher claim acceptance rates
- Faster reimbursements
- Reduced staffing costs
- Access to billing experts
For growing practices, working with the best outsource mental health billing and coding services can be a game-changer.
When Should You Consider Outsourcing?
- Frequent claim denials
- Limited in-house expertise
- Rapid practice growth
- Difficulty keeping up with regulatory changes
Choosing the Right Mental Health Billing Solutions
Not all billing providers are created equal. Selecting the right mental health billing solutions can significantly impact your financial performance.
What to Look For:
- Experience in behavioral and mental health billing services
- Transparent pricing models
- Strong reporting and analytics
- Compliance with HIPAA regulations
- Integration with your EHR system
Avoid choosing solely based on cost—even a cheap outsource mental health billing company can end up costing more due to errors.
Real-World Example: A Growing Therapy Practice
Consider a mid-sized therapy clinic in Texas that struggled with delayed reimbursements and high denial rates. Their in-house team lacked expertise in billing for mental health services, leading to inefficiencies.
After switching to outsourced billing for mental health:
- Claim acceptance improved by 30%
- Revenue increased within 3 months
- Administrative workload reduced significantly
This shift allowed therapists to focus more on patient care instead of paperwork.
Integrating Revenue Cycle Management for Better Results
Effective billing is part of a larger system known as revenue cycle management services. This approach covers every financial interaction from patient intake to final payment.
Key Stages:
- Patient registration
- Insurance verification
- Charge capture
- Claims submission
- Payment posting
- Reporting and analytics
When properly implemented, RCM ensures consistent cash flow and financial stability.
The Importance of Medical Billing and Coding Services
Mental health practices benefit greatly from specialized medical billing and coding services. These services ensure:
- Compliance with evolving regulations
- Accurate coding practices
- Reduced audit risks
- Improved financial performance
Pairing billing with expert medical coding services creates a seamless workflow that minimizes errors and maximizes reimbursements.
Common Mistakes in Billing for Mental Health
Even experienced providers can make costly errors. Here are some pitfalls to avoid:
- Incorrect session time coding
- Missing documentation
- Failure to verify insurance
- Delayed claim submission
- Ignoring denied claims
Addressing these issues early can save both time and revenue.
Future Trends in Mental Health Billing
The landscape of billing services for mental health clinics is evolving rapidly.
Emerging Trends:
- Increased use of AI in claim processing
- Expansion of telehealth billing
- Value-based care models
- Enhanced data analytics
Staying ahead of these trends can give providers a competitive advantage.
Final Thoughts
Billing for mental health is more than just submitting claims—it’s a strategic function that directly impacts the success of your practice. From accurate coding to efficient claims management, every step plays a role in maintaining financial health.
For practices looking to scale or reduce administrative burden, partnering with experienced providers like 247 medical billing services can make a meaningful difference. By combining expertise in medical billing services, medical coding services, and comprehensive revenue cycle management services, along with reliable credentialing services, providers can focus on what truly matters—delivering quality mental health care.
FAQs
1. What is the biggest challenge in billing for mental health?
The biggest challenge is managing complex coding requirements and varying insurance policies, which often lead to claim denials if not handled properly.
2. Should mental health providers outsource billing?
Outsourcing can be highly beneficial, especially for growing practices, as it improves accuracy, reduces workload, and speeds up reimbursements.
3. How does credentialing affect mental health billing?
Without proper credentialing, providers cannot bill insurance companies, making it a critical step in the billing process.
4. What are common codes used in mental health billing?
Common CPT codes include 90791, 90834, and 90837, while ICD-10 codes vary based on diagnoses like anxiety or depression.
5. Is Medicare billing different for mental health services?
Yes, Medicare has strict guidelines regarding medical necessity, documentation, and provider eligibility.
6. How can practices improve their billing efficiency?
Implementing strong revenue cycle management, using accurate coding practices, and considering outsourced billing solutions can significantly improve efficiency.